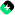Coverage Limitations for Ketamine Services Under Blue Cross Blue Shield
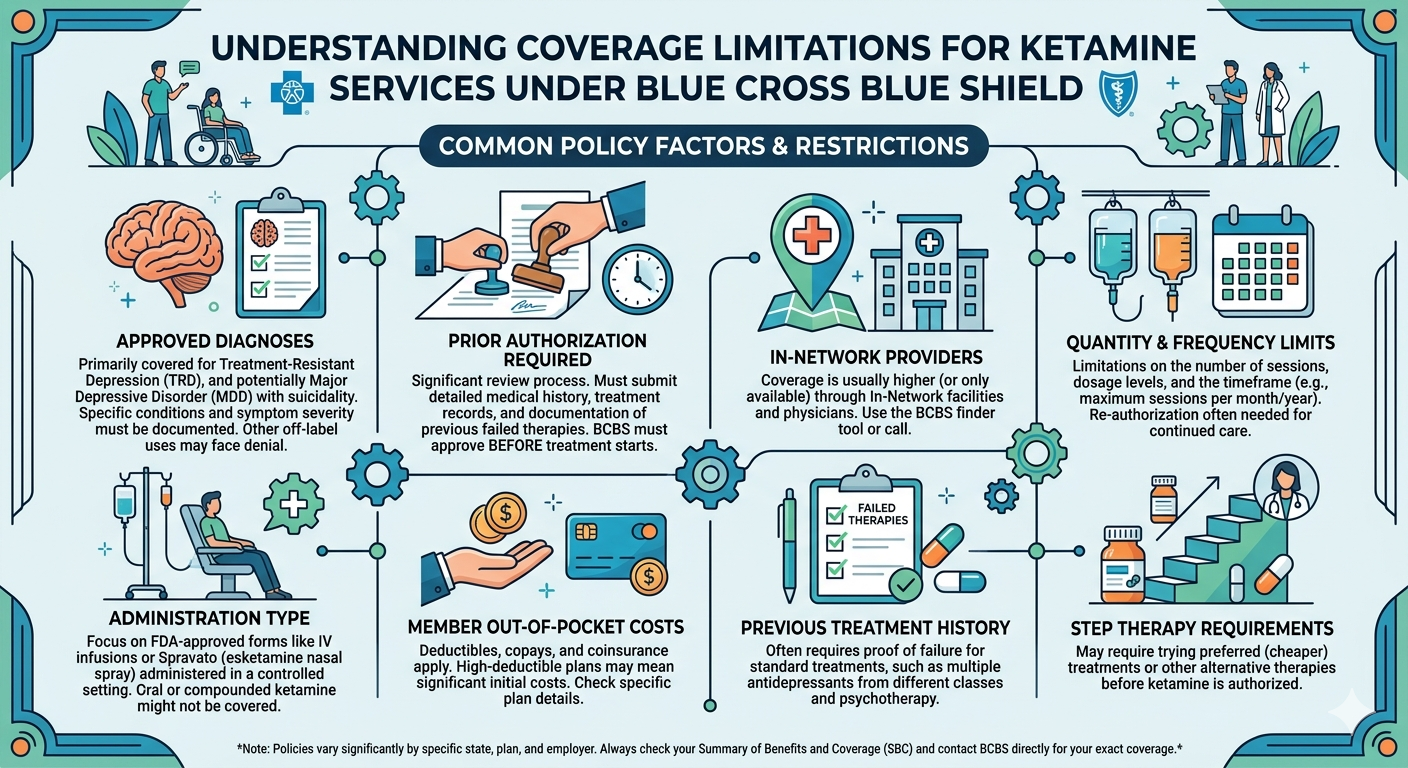
Ketamine therapy has emerged as a groundbreaking treatment for individuals with depression, anxiety, and other mood disorders, offering a new hope for those who have not found relief through traditional medications. However, despite its growing popularity, many patients are left wondering about the financial aspects of ketamine therapy, particularly when it comes to insurance coverage. One of the most frequently asked questions is: Does Blue Cross Blue Shield cover ketamine treatment?
In this article, we’ll explore the insurance coverage limitations for ketamine services under Blue Cross Blue Shield (BCBS). We’ll discuss what you need to know about coverage, how the insurance company determines eligibility, and what steps you can take to navigate the challenges of seeking ketamine therapy through your health plan.
Understanding Ketamine as a Treatment for Mental Health
Ketamine was originally developed as an anesthetic but has since gained attention for its fast-acting antidepressant effects, especially for individuals suffering from treatment-resistant depression, post-traumatic stress disorder (PTSD), and severe anxiety. Traditional antidepressants, such as selective serotonin reuptake inhibitors (SSRIs), often take weeks to show results, but ketamine offers relief in as little as 24 to 72 hours. This rapid onset has made it a game-changer for patients who need quick relief from debilitating symptoms.
However, despite its effectiveness, ketamine treatment remains classified as an off-label use for mental health disorders, which presents challenges when it comes to insurance coverage. Blue Cross Blue Shield, one of the largest health insurance providers in the United States, is often the go-to provider for many individuals, but whether or not Blue Cross Blue Shield covers ketamine treatment can vary depending on several factors.
Insurance Coverage and the Challenges of Ketamine Therapy
As of now, ketamine therapy is not widely covered under most insurance plans, including Blue Cross Blue Shield, except in specific circumstances. Generally, BCBS will not provide coverage for off-label treatments unless there is substantial evidence and documentation that the treatment is medically necessary. For ketamine, this means that BCBS may only cover the therapy if it is part of a clinical trial or if the treatment is being administered in a hospital or medical setting under the supervision of a licensed healthcare professional.
Many individuals who pursue ketamine therapy for mental health conditions do so through clinics that offer infusion treatments or nasal spray forms of ketamine. These clinics typically operate outside of the hospital setting, making it difficult to qualify for insurance reimbursement. Therefore, for most patients, ketamine therapy under BCBS will likely be considered out-of-pocket, and the costs can be significant. A single infusion session can range from $400 to $800, depending on the clinic and location, and patients typically require several sessions for optimal results.
Coverage Limitations: What Does Blue Cross Blue Shield Cover?
So, does Blue Cross Blue Shield cover ketamine treatment? It depends. BCBS offers several different health plans, and the coverage for ketamine therapy can vary depending on your specific plan, your healthcare provider’s network, and the medical necessity of the treatment.
Here’s what you need to know about coverage limitations:
1. Off-Label Use and Coverage for Mental Health Conditions
Most insurance companies, including BCBS, are hesitant to cover treatments for mental health conditions that are not FDA-approved. Ketamine is considered an off-label treatment for depression, PTSD, and anxiety, which means it is not officially recognized by the FDA as a standard treatment for these conditions. As a result, BCBS may not cover ketamine therapy unless you can demonstrate that other conventional treatments, such as SSRIs, have failed and that ketamine is medically necessary for your condition.
2. Hospital vs. Outpatient Treatment
If you’re receiving ketamine treatment in a hospital setting, BCBS is more likely to consider it for reimbursement, especially if you’re participating in a clinical trial or under the supervision of an experienced healthcare provider. However, ketamine is often administered at outpatient clinics, which may not meet the requirements for insurance reimbursement. In these cases, the cost of treatment will likely fall on the patient, unless your plan offers specific coverage for outpatient mental health treatments.
3. Clinical Trials and Research-Based Coverage
Some individuals may be able to access ketamine therapy under BCBS if they are enrolled in a clinical trial or research study. In these cases, Blue Cross Blue Shield may provide coverage if the treatment is part of a legitimate medical study or trial. These studies are often conducted at academic medical centers or research facilities, where ketamine treatment is being studied for its effects on mental health. Patients involved in such studies may have access to ketamine therapy at little or no cost, with the potential for insurance reimbursement depending on the specifics of the trial.
4. Appeals Process for Denied Claims
If your claim for ketamine treatment is denied, it’s important to know that you have the right to appeal the decision. Insurance providers, including BCBS, must allow you to challenge denied claims if you believe the treatment is medically necessary. In some cases, a letter from your doctor outlining the necessity of ketamine treatment, along with supporting documentation of your medical history and failure to respond to traditional therapies, can help your case. Working closely with your healthcare provider and BCBS representatives can help you navigate the appeals process more effectively.
What You Can Do to Improve Your Chances of Coverage
While Blue Cross Blue Shield coverage for ketamine treatment remains limited, there are steps you can take to improve your chances of receiving reimbursement or to reduce your out-of-pocket expenses:
1. Work with Your Doctor
Your healthcare provider can be your strongest ally in securing coverage for ketamine therapy. They can provide a detailed medical record that shows why ketamine is the right choice for your treatment and why other methods have failed. The more documented evidence your provider can supply, the better your chances of approval.
2. Contact Blue Cross Blue Shield Directly
Reach out to BCBS customer service to ask about your specific policy’s coverage for ketamine treatment. Ask for clarification on whether they will reimburse ketamine services under any circumstances, especially in cases of treatment-resistant depression. It’s essential to understand what your policy covers and how to present your case to BCBS.
3. Explore Other Financial Assistance Options
Some ketamine clinics offer financing plans or sliding-scale fees to help patients who cannot afford the full cost of treatment. Additionally, some organizations and nonprofits may provide grants or financial assistance to those seeking ketamine therapy for mental health conditions.
Conclusion
While Blue Cross Blue Shield does not widely cover ketamine treatment, there may still be avenues for reimbursement depending on the specific circumstances of your case. It’s important to work closely with your healthcare provider, understand the limitations of your policy, and consider other financial assistance options to help offset the cost. As the use of ketamine for mental health continues to grow, it’s likely that insurance providers, including BCBS, will continue to reassess their coverage policies. Until then, being proactive and informed about your insurance options can help you navigate the financial challenges of seeking ketamine therapy.
If you are struggling with depression or other mood disorders, consult with your healthcare provider to explore the potential of ketamine therapy and how it can fit into your treatment plan.